Blog
Subscribe To The Purview Blog
-

Reflections from the American Association of Legal Nurse Consultants 2026 Annual Conference in Orlando
[Litigation]Read Now -

Beyond the Zip Code: When Expertise Isn’t Local, Access Can’t Be Either
[Second Opinions]Read Now -

How Legal Nurse Consultants Transform Cases
[Litigation]Read Now -

How Animalius Grew—and Why They Switched to Purview
[Vets/Equine, veterinary medicine]Read Now -

Why Payers and Employers Invest in Second Opinions for High-Stakes Medical Decisions
[Healthcare Technology]Read Now -

The Imaging Access Problem That Slows Down Subspecialty Care
[Healthcare Technology]Read Now -

Why Most US Providers Require English Translation of International Medical Records
[Second Opinions, international]Read Now -

Cross-Border Telehealth: Why Data Residency Can Make or Break Remote Access
[Second Opinions, Compliance/Legislation]Read Now -

The Second-Opinion Liability Myth: What Concierge Firms Don’t Always Tell You
[Second Opinions, Compliance/Legislation]Read Now -
What's the Difference Between a Concierge Led Second Opinion Program & Establishing Our Own?
[Second Opinions, Concierge]Read Now -

Why Remote Access to Medical Images Has Become A Vital Part of Horse Racing and Auctions
[Vets/Equine, veterinary medicine]Read Now -

Has My Veterinary Practice Outgrown Horos?
[Vets/Equine, veterinary medicine]Read Now -

How Medical Imaging Can Play a Role in Gaining Expert Certification for Personal Injury and Medical Malpractice Cases
[Litigation]Read Now -

Presenting Medical Images as Evidence; A Strategic Advantage in Trial
[Medical Imaging, Healthcare Technology, Litigation]Read Now -

Top 10 Horos Questions - Answered
[Horos]Read Now -
%20wp-content/2017/11/ViVA-for-Vet_Viewer-Images-1024x583.png?height=200&name=ViVA-for-Vet_Viewer-Images-1024x583.png)
How Vets Who Use Horos Store, Share, and Report
[Cloud PACS, Vets/Equine]Read Now -

Four Compelling Reasons To Incorporate Medical Images in Malpractice or Personal Injury Lawsuits
[Medical Imaging, Litigation]Read Now -

I’m a Provider. Can I Give Consults to Patients Outside of My State?
[Remote/Consulting Radiology, Hospitals, Second Opinions, Compliance/Legislation, Healthcare Technology, Oncology]Read Now -

What is the REAL COST of burning a CD/DVD every time you want to share medical images?
[Compliance/Legislation, Litigation]Read Now -

Clarity in the Courtroom: The Power of DICOM Imaging in Malpractice and Personal Injury Litigation
[Medical Imaging, Litigation]Read Now -

The Visual Verdict: DICOM vs. JPG Images in Legal Proceedings
[Medical Imaging, Compliance/Legislation, Litigation]Read Now -

What's New With Expert View? Watch the latest and greatest celebrated features within Purview's market leading second opinion software
[Second Opinions, Healthcare Technology]Read Now -

When is a patient a patient?
[Hospitals, Second Opinions, Patient Transfers, Compliance/Legislation, Policy, Licensure, HIPAA]Read Now -
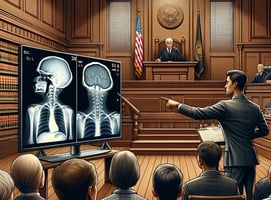
Lawyers Handling Medical DICOM Images for Litigation; How to get the most value from evidence without risking a HIPAA violation
[Medical Imaging, Litigation]Read Now -

Horos & Purview Image - What’s the Difference?
[Medical Imaging, Cloud PACS, Healthcare Technology]Read Now -

Navigating Turbulent Legal Waters: HIPAA Responsibilities for Lawyers Handling Private Health Information in Litigation
[Compliance/Legislation, Litigation, HIPAA]Read Now -
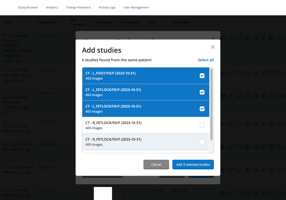
How to Share Multiple Studies Simultaneously
[Medical Imaging, Cloud PACS, Healthcare Technology]Read Now -
Why Having a Physician Licensed in Every Jurisdiction Doesn’t Completely Satisfy Licensure Regulations
[Hospitals, Second Opinions, Compliance/Legislation, Litigation, Licensure]Read Now -
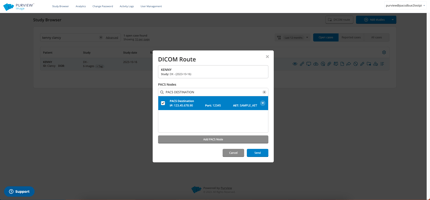
Will the DICOM Router Save Me Time?
[Medical Imaging, Cloud PACS, Healthcare Technology]Read Now -

8 Ways to Use Purview Image™ That Might Surprise You
[Imaging Centers, Medical Imaging, Cloud PACS]Read Now -

Will Moving Your Cloud PACS Back On-Site Really Save You Money?
[Imaging Centers, Medical Imaging, Remote/Consulting Radiology, Cloud PACS]Read Now -

Doctor on Deck: How Health Workers Can Take a Break
[]Read Now -
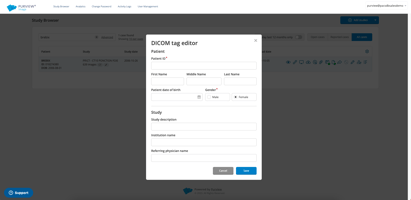
Mastering DICOM Editing for Research & Education
[Medical Imaging, Cloud PACS, Healthcare Technology]Read Now -

The Boundaries of Horos: Key Takeaways from the Webinar
[Medical Imaging, Cloud PACS, Healthcare Technology]Read Now -

Unraveling Cross-State Licensure For Second Opinions: Highlights From The Live Q&A Discussion
[Compliance/Legislation, Policy, Licensure]Read Now -

How Far Can Horos Go? What To Do When Working With Limited Sharing, Access, and Mobility
[Medical Imaging, Cloud PACS, Healthcare Technology]Read Now -

Preventing Catastrophic Outcomes at the Track - We Can Do Better
[]Read Now -

Second Opinions for Children - An Interview with Dr. Jesse Skoch, Neurosurgeon at Cincinnati Children's Hospital
[Second Opinions]Read Now -

Dr. Schwaab of Roswell Park Comprehensive Cancer Center, On Second Opinions for Cancer Patients
[Specialists, Second Opinions, Oncology, pathology]Read Now -
Online Pre-Surgical Reviews: A Step Towards Improving Patient and Physician Experience Along With Throughput, That Everyone Can Get Behind
[Hospitals, Second Opinions, Healthcare Technology, asynchronous, payers]Read Now -

Can Physicians Really Work From Anywhere?
[Cloud PACS]Read Now -

Race to the Top with Purview Image: Streamline the Review of a Horse's Medical History
[Vets/Equine]Read Now -

The Legal Reality of Issuing Second Opinions for Out of State Patients
[Remote/Consulting Radiology, Hospitals, Second Opinions, Compliance/Legislation, Healthcare Technology]Read Now -

Work Smarter, Not Harder with a Cloud PACS
[Medical Imaging, Cloud PACS, Healthcare Technology]Read Now -

Ready to Launch Your Second Opinion Program? What to Expect When Preparing for 'Go-Live'
[Hospitals, Second Opinions, Healthcare Technology]Read Now -
Design for Better Health Care - Are We There Yet?
[Healthcare Technology, Patient Experience, payers]Read Now -

Collaboration - A Modern Necessity For Targeted Cancer Treatment?
[Second Opinions, Oncology]Read Now -

Second Opinion Guidance for Families from Cincinnati Children's Hospital & Dr. Skoch
[Hospitals, Second Opinions, Neuro]Read Now -

Serving Out of State Patients? The 2023 Post-Pandemic, Post-PHE Update
[Specialists, Second Opinions, Compliance/Legislation]Read Now -

Why Asynchronous Part 3; Benefits for Payers
[Second Opinions, asynchronous, payers]Read Now -
Why Asynchronous Part 2; Provider Benefits & Opportunities
[Second Opinions, Healthcare Technology, asynchronous]Read Now -

Why Asynchronous Part 1; Patient Benefits
[Second Opinions, Healthcare Technology, asynchronous]Read Now -

Is Your Hospital Ready for a Second Opinion Program?
[Specialists, Hospitals, Second Opinions, Healthcare Technology, Patient Experience]Read Now -

'It's Cancer - Now what?'
[Patients]Read Now -
.png?height=200&name=_Blog%20Graphics%20(63).png)
Structured Reporting vs. DICOM Structured Reporting
[Medical Imaging, Cloud PACS, Healthcare Technology]Read Now -

The Top 10 Hottest Purview Blogs of 2022
[Second Opinions, Healthcare Technology, pathology, orthopedics]Read Now -
Applying Data Science to Healthcare
[]Read Now -
Why Children’s Hospitals Need a Remote Second Opinion Program Right Now
[Hospitals, Second Opinions, Healthcare Technology]Read Now -
Are Remote Second Opinions an Option in Orthopedics?
[Second Opinions, orthopedics]Read Now -
A Medical Imaging Cloud PACS for Equine Veterinarians Enables Mobility
[]Read Now -

The Critical Role of Foundations and Not-for-Profits in the Patient Provider Relationship
[Mike Shane Memorial Fund]Read Now -

What do we mean when we say 'adaptive services' and how can they help?
[Healthcare Technology, Patient Experience]Read Now -

A Step-by-Step Guide to Getting a Second Opinion
[Second Opinions, Patients]Read Now -

Thoughtful Automation in the Patient Experience; Lessons from Other Industries
[Healthcare Technology, Patient Experience]Read Now -
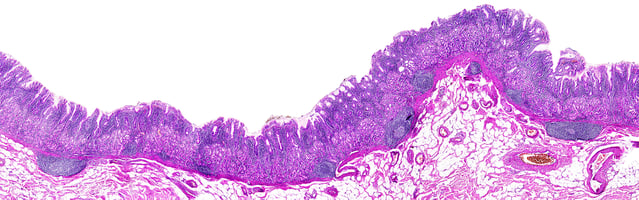
Pathology Second Opinions - Look Again
[Second Opinions, pathology]Read Now -

7 Tips for Marketing Your Second Opinion Program
[Second Opinions]Read Now -

Welcome to the 'Virtual Front Door'
[Second Opinions, Patient Experience]Read Now -

Are Medical Second Opinions Profitable?
[Second Opinions]Read Now -

The Case for Multidisciplinary Review During Remote Second Opinions
[Second Opinions, Oncology]Read Now -

When to Seek A Second Opinion for Your Child
[Second Opinions, Patients]Read Now -

Five Reasons Why Your Hospital’s Second Opinion Program Is Not Growing
[Second Opinions, Concierge]Read Now -

When Your Child is Diagnosed with Cancer - Second Opinions Can Provide Clarity and Guidance
[Patients]Read Now -
.png?height=200&name=Untitled%20(600%20%C3%97%20250%20px).png)
Managing Risk in 'Curbside Consults': Systematize, Legalize & Monetize Your Second Opinion Program
[Hospitals, Second Opinions, Compliance/Legislation, Healthcare Technology]Read Now -
What Happens If I Lose My Patient's Medical Images?
[Imaging Centers, Medical Imaging, Security, Cloud PACS, Compliance/Legislation, Healthcare Technology]Read Now -
Uniform Telehealth Act Provides Stunning Enablement of Consults Across State Lines
[Second Opinions, Compliance/Legislation]Read Now -

Attracting International Second Opinion Patients
[]Read Now -

10 Ways to Internally Market Your Second Opinion Program
[Second Opinions]Read Now -

Can I Ask My Doctor to Get Me A Second Opinion?
[Patients]Read Now -

For a Cloud PACS, How Fast Does My Internet Access Need to Be?
[]Read Now -

How Can I Use Telehealth to Reach Rural Patients?
[Specialists, Remote/Consulting Radiology, Hospitals, Second Opinions, Compliance/Legislation, Healthcare Technology, Oncology, Chiro, Cardio, Neuro]Read Now -

Second Opinion Programs: What About Physician Burnout?
[Specialists, Hospitals, Second Opinions, Healthcare Technology, Oncology]Read Now -

Sharing Medical Records with Expert Witnesses: A Guide for Legal Professionals
[Litigation]Read Now -

How Much Does Purview Software Cost?
[Medical Imaging, Remote/Consulting Radiology, Hospitals, Second Opinions, Cloud PACS, Healthcare Technology]Read Now -
.png?height=200&name=_Blog%20Graphics%20(51).png)
How Do I Upload Scans to the Cloud From My Modality?
[Imaging Centers, Specialists, Remote/Consulting Radiology, Cloud PACS, Healthcare Technology]Read Now -
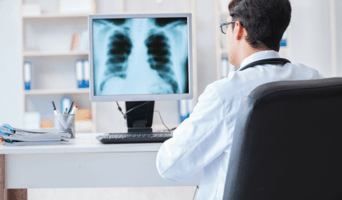
Horos vs. Purview - What's the difference?
[]Read Now -

Remote Second Opinions: A Cure for the C-suite Blues
[Hospitals, Second Opinions]Read Now -

Why Not Every Hospital Should Consider a Virtual Second Opinion Program
[Hospitals, Second Opinions]Read Now -
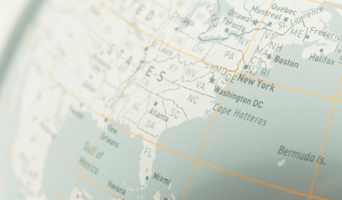
Practicing Medicine Beyond Your Own State's Border
[Specialists, Hospitals, Second Opinions]Read Now -

Is Dropbox HIPAA Compliant for Medical Imaging?
[Imaging Centers, Specialists]Read Now -

How to Drive Patient Engagement with Remote Consults
[]Read Now -

Concierge vs Software & Services: Which One is Best for My Organization?
[Hospitals, Second Opinions, Healthcare Technology]Read Now -
.png?height=200&name=64%20(1).png)
Purview Lite vs. Purview Image: What’s the Difference?
[]Read Now -

Is Cloud Storage Right for My Medical Imaging Modality?
[Imaging Centers, Specialists, Medical Imaging, Cloud PACS, Healthcare Technology, Vets/Equine]Read Now -

Delivering the Future of Healthcare: Do Remote Second Opinions Open New Doors?
[]Read Now -

Should I Compress DICOM Images? Optimizing Medical Images
[Imaging Centers, Remote/Consulting Radiology, Security, Cloud PACS, Healthcare Technology]Read Now -
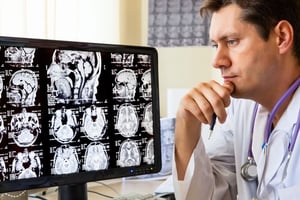
How Can Patients Send an Existing DICOM Medical Imaging Study?
[Imaging Centers, Specialists, Medical Imaging, Remote/Consulting Radiology, Cloud PACS, Healthcare Technology]Read Now -

6 Questions to Avoid a PACS Data Backup Disaster in 2022 | Purview
[Imaging Centers, Cloud PACS, Healthcare Technology]Read Now -

How to Charge Patients for Copies of their Medical Images, According to HIPAA
[Imaging Centers, Medical Imaging, Compliance/Legislation]Read Now -

Synchronous vs Asynchronous Communication in Telemedicine | Purview
[Hospitals, Second Opinions, Healthcare Technology, Oncology, Pain Management (brain/spine/pain), Chiro, Cardio, Neuro]Read Now -

How to Avoid No-Shows and Cancellations at Your Medical Practice
[Imaging Centers, Specialists, Remote/Consulting Radiology, Hospitals, Healthcare Technology, Vets/Equine, Oncology, Pain Management (brain/spine/pain), Chiro, Neuro]Read Now -

How to Ensure HIPAA Compliance with Image Sharing in 2022
[Medical Imaging, Compliance/Legislation]Read Now -
.png?height=200&name=image%20(1).png)
8 Healthcare Recruitment Strategies for Attracting and Retaining Top Talent
[Specialists, Hospitals, Healthcare Technology, Oncology]Read Now -

Does Medicaid Cover Second Opinions in 2022?
[Mike Shane Memorial Fund, Hospitals, Second Opinions, Compliance/Legislation]Read Now -

What is a Remote Second Opinion (RSO)?
[Specialists, Hospitals, Second Opinions, Healthcare Technology, Oncology, Neuro]Read Now -

How Much Does a New PACS Cost?
[Medical Imaging, Cloud PACS, Healthcare Technology]Read Now -

Second Opinion Program: Should I do a Proof of Concept?
[Hospitals, Second Opinions, Healthcare Technology]Read Now -
.png?height=200&name=_Blog%20Graphics%20(62).png)
What is a DICOM Uploader?
[Imaging Centers, Medical Imaging, Remote/Consulting Radiology, Healthcare Technology]Read Now -
.png?height=200&name=_Blog%20Graphics%20(60).png)
Can I Attract New Patients with Second Opinions?
[Second Opinions]Read Now -
.png?height=200&name=_Blog%20Graphics%20(59).png)
Does Virtual Care Create a Better Experience for Patients?
[Specialists, Hospitals, Second Opinions, Healthcare Technology, Oncology]Read Now -
-1.png?height=200&name=_Blog%20Graphics%20(13)-1.png)
Can my Cloud PACS Integrate with my Existing Systems?
[Medical Imaging, Cloud PACS, Healthcare Technology]Read Now -
-png.png?height=200&name=_Blog%20Graphics%20(58)-png.png)
Medical Records Requests: What to Expect
[Patients]Read Now -
-1.png?height=200&name=_Blog%20Graphics%20(11)-1.png)
Advice For Newly Diagnosed Cancer Patients
[Patients]Read Now -
.png?height=200&name=_Blog%20Graphics%20(57).png)
My Summer Internship Experience
[]Read Now -
-1.png?height=200&name=_Blog%20Graphics%20(10)-1.png)
Are Purview Solutions Secure?
[Security, Healthcare Technology]Read Now -

Which Purview Solution is Right for Me?
[Imaging Centers, Specialists, Medical Imaging, Hospitals, Second Opinions, Cloud PACS, Healthcare Technology, Oncology, Pain Management (brain/spine/pain), Chiro, Cardio, Neuro]Read Now -

Horos vs. OsiriX: What's the Difference?
[Medical Imaging, Healthcare Technology, Vets/Equine]Read Now -
-1.png?height=200&name=_Blog%20Graphics%20(9)-1.png)
Should I Move Legacy DICOM Data To The Cloud?
[Medical Imaging, Cloud PACS]Read Now -
-1.png?height=200&name=_Blog%20Graphics%20(7)-1.png)
How Can I Get a Second Opinion Without Traveling?
[Patients]Read Now -

Navigating the Legal Minefield of Collecting Medical Records
[Litigation]Read Now -
-1.png?height=200&name=_Blog%20Graphics%20(4)-1.png)
Common Problems When Changing from a Local to a Cloud PACS
[Medical Imaging, Cloud PACS, Healthcare Technology]Read Now -
-1.png?height=200&name=_Blog%20Graphics%20(6)-1.png)
How Can I Measure the Success Of My Telehealth Program?
[Hospitals, Second Opinions, Healthcare Technology]Read Now -
-1.png?height=200&name=_Blog%20Graphics%20(8)-1.png)
Purview's 8 Golden Standards of Account Management
[Healthcare Technology]Read Now -
-1.png?height=200&name=_Blog%20Graphics%20(5)-1.png)
Is Purview Image Customizable?
[Medical Imaging, Cloud PACS, Healthcare Technology]Read Now -
.png?height=200&name=_Blog%20Graphics%20(54).png)
Can I Lose Medical Images in a Cloud PACS?
[Security, Cloud PACS, Healthcare Technology]Read Now -

How to Access DICOM Data From Multiple Locations
[Imaging Centers, Medical Imaging, Remote/Consulting Radiology, Hospitals, Cloud PACS, Healthcare Technology]Read Now -
-1.png?height=200&name=_Blog%20Graphics%20(2)-1.png)
How Can I Manage Patient Cases More Effectively?
[Hospitals, Second Opinions, Patient Transfers, Healthcare Technology, Oncology]Read Now -
-1.png?height=200&name=_Blog%20Graphics%20(1)-1.png)
How Can I Grow My Mobile Radiology Practice?
[]Read Now -
.png?height=200&name=_Blog%20Graphics%20(52).png)
Account Management vs Customer Support
[]Read Now -
.png?height=200&name=_Blog%20Graphics%20(50).png)
DICOM Troubleshooting: Is the Metadata Compliant?
[Medical Imaging, Cloud PACS, Healthcare Technology]Read Now -
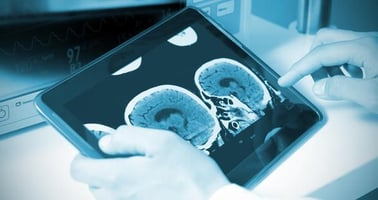
How Can I View DICOM Images Remotely?
[Specialists, Medical Imaging, Remote/Consulting Radiology, Second Opinions, Cloud PACS, Healthcare Technology]Read Now -
.png?height=200&name=_Blog%20Graphics%20(48).png)
Can You Email Medical Records?
[Security, Cloud PACS, Compliance/Legislation, Healthcare Technology]Read Now -

How Can I Start Offering Second Opinions?
[Hospitals, Second Opinions]Read Now -
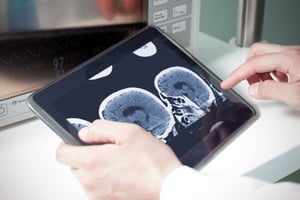
How Much Does a Cloud PACS Cost?
[Medical Imaging, Cloud PACS]Read Now -
Oncology Second Opinion vs. Tumor Board Review: What's the Difference?
[Patients]Read Now -
.png?height=200&name=_Blog%20Graphics%20(45).png)
How Much Should My Second Opinion Program Budget Be?
[Hospitals, Second Opinions]Read Now -
.png?height=200&name=_Blog%20Graphics%20(44).png)
5 Reasons to Start a Second Opinion Program
[Hospitals, Second Opinions]Read Now -

3 Reasons You Should Charge Your Patients for Access to Their Medical Images
[Imaging Centers]Read Now -
.png?height=200&name=_Blog%20Graphics%20(42).png)
How Online Second Opinions Can Help You Harness Your Hospital's Brand
[]Read Now -
.png?height=200&name=_Blog%20Graphics%20(14).png)
The Ultimate Guide to Getting a Second Opinion
[Patients]Read Now -
.png?height=200&name=_Blog%20Graphics%20(37).png)
Where We Stand on the Cures Act
[]Read Now -
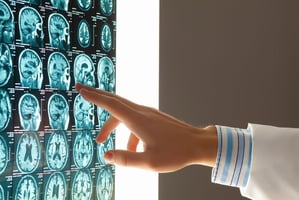
Why Specialist Doctors Shouldn't Rely on a Hospital PACS
[]Read Now -
.png?height=200&name=_Blog%20Graphics%20(36).png)
How to Get Paid for Remote Expert Opinions
[]Read Now -
-png.png?height=200&name=_Blog%20Graphics%20(35)-png.png)
Connection to Core Systems for Remote Second Opinion Programs
[]Read Now -
.png?height=200&name=_Blog%20Graphics%20(33).png)
How Can I Share My Patients' Medical Records for a Second Opinion?
[]Read Now -
.png?height=200&name=_Blog%20Graphics%20(31).png)
What Resources Do I Need to Start a Remote Second Opinion Program?
[]Read Now -
.png?height=200&name=_Blog%20Graphics%20(28).png)
Build vs Buy: Enterprise Medical Software
[]Read Now -
.png?height=200&name=_Blog%20Graphics%20(24).png)
Strategies for Improving Medical Record Exchange for Patient Transfer
[]Read Now -
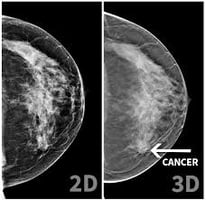
The Importance of Getting a Second Opinion on Breast Cancer
[Patients]Read Now -
.png?height=200&name=_Blog%20Graphics%20(23).png)
Which Telehealth Services Should My Organization be Offering?
[]Read Now -
.png?height=200&name=_Blog%20Graphics%20(22).png)
How to Collect a Complete Set of Patient Records Prior to a Consult
[]Read Now -
.png?height=200&name=_Blog%20Graphics%20(19).png)
How Can I Aggregate Medical Records Within My Patient Intake Software?
[]Read Now -
.png?height=200&name=_Blog%20Graphics%20(18).png)
Should I Hire an Administrator for Remote Second Opinions (RSOs)?
[]Read Now -
-png.png?height=200&name=_Blog%20Graphics%20(15)-png.png)
How Do I Obtain My Loved One's Medical Records?
[]Read Now -
.png?height=200&name=_Blog%20Graphics%20(13).png)
How to Collect Your Medical Records for a Clinical Trials
[]Read Now -
.png?height=200&name=_Blog%20Graphics%20(11).png)
How Can Patients Send Physicians an Existing Pathology Report?
[]Read Now -

2020 Roundup - Ten Healthcare Trends That We Believe are Here to Stay
[]Read Now -
.png?height=200&name=_Blog%20Graphics%20(10).png)
Looking For a Charity to Support this #GivingTuesday? Look No Further
[Mike Shane Memorial Fund]Read Now -
.png?height=200&name=_Blog%20Graphics%20(7).png)
5 Things Imaging Centers Should Eliminate From Their Workflow
[Imaging Centers]Read Now -
.png?height=200&name=_Blog%20Graphics%20(3).png)
AnimalScan: A Journey to Becoming Experts in Animal Imaging
[]Read Now -
Remote Second Opinions: An Important Tool in Your Virtual Care Toolbox
[]Read Now -

The Best Way to Collect Patient Records from Various Providers
[]Read Now -

3 Strategies for Imaging Practices to Grow in Times of COVID-19
[]Read Now -
.png?height=200&name=Untitled%20design%20(8).png)
Littrell Radiology provides timely chiropractic radiological reads
[Specialists, Chiro]Read Now -
.png?height=200&name=Untitled%20design%20(9).png)
How Tungsten Medical Network Delivers on Quality and Service for ENT Practices
[Specialists, Cloud PACS]Read Now -
.png?height=200&name=Untitled%20design%20(10).png)
How Diagnostic Imaging is Safely Spreading the Word About Patient Access
[Imaging Centers]Read Now -

How Diagnostic Imaging Reduced Costs and Increased Patient Satisfaction
[Imaging Centers]Read Now -

How South American Health Care Practices Continue to Work Safely During COVID-19
[]Read Now -

The ROI of Remote Second Opinions
[Specialists, Hospitals, Second Opinions]Read Now -

Our Commitment to Customer Service
[]Read Now -

How Patient Perspectives on Telehealth are Changing
[Healthcare Technology]Read Now -

5 Steps to Offering Remote Second Opinions for Subspecialists
[]Read Now -

How primary care physicians need to adapt to reach millennials
[]Read Now -
%20(1).png?height=200&name=Free%20Image%20Sharing%20Service%20Info%20graphics%20(2)%20(1).png)
Spotlight: How do physicians use Telehealth during coronavirus?
[]Read Now -

Should my subspecialist practice offer remote second opinions?
[]Read Now -

Is my hospital prepared to offer remote second opinions?
[Hospitals, Second Opinions]Read Now -

How can my hospital choose the best software for a remote or second opinion service?
[Hospitals, Second Opinions]Read Now -

Should hospitals offer a remote second opinion service?
[]Read Now -
.png?height=200&name=Free%20Image%20Sharing%20Service%20Info%20graphics%20(2).png)
Spotlight: How can physicians and veterinarians use Telehealth during coronavirus?
[]Read Now -

What telemedicine software is best for remote second opinions?
[Hospitals, Second Opinions]Read Now -

What funding opportunities are available for healthcare institutions to get Telehealth?
[]Read Now -

How are providers using Purview's Telehealth services during coronavirus?
[]Read Now -
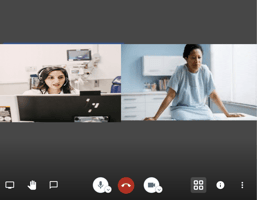
What is telemedicine and what type is best for my organization?
[]Read Now -

How has coronavirus changed Medicare coverage for Telehealth services?
[]Read Now -
.png?height=200&name=Free%20Image%20Sharing%20Service%20(2).png)
Share Medical Images Safely During COVID-19 Pandemic
[]Read Now -

Will Older Patients Use an App for Medical Image Access?
[]Read Now -

Is There A Mobile App To Access Patient Medical Imaging?
[]Read Now -
.png?height=200&name=Untitled%20design%20(6).png)
Patients Can Share Medical Images Without Delays or Costs to Providers
[Imaging Centers, Specialists]Read Now -

Improve Medical Outcomes with Online Patient Access to Medical Images
[Imaging Centers, Specialists]Read Now -

3 Reasons Why CDs are Obsolete in Medical Imaging
[]Read Now -

Access to Medical Images: Are You Meeting Your Patients' Expectations?
[Imaging Centers, Specialists]Read Now -

Online Access to Medical Images Benefits Cholangiocarcinoma Patients
[Mike Shane Memorial Fund]Read Now -

Patients Prefer Self-Pay for Copies of Their Medical Images
[]Read Now -

Yale Researchers Warn Hospitals: Using CDs for Patient Image Delivery is 'Immediate Issue'
[Imaging Centers, Specialists]Read Now -
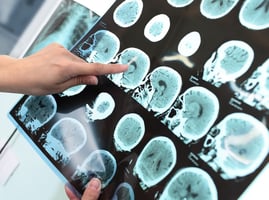
Should Patients Have Access to Medical Images?
[Imaging Centers, Specialists]Read Now -

Deliver Patient Access to Medical Images Without Using CDs
[Imaging Centers, Specialists]Read Now -

Smartphones are Changing the Way Patients Access Medical Images
[Imaging Centers, Specialists]Read Now -

A Breast Cancer Survivor’s Perspective on Second Opinions
[Patients, Oncology]Read Now -
.png?height=200&name=_Blog%20Graphics%20(41).png)
Four Steps for a More Efficient Clinical Trial
[]Read Now -

3 Benefits of Giving Your Patients Self-Service Access to Mammograms
[Imaging Centers, Specialists, Oncology]Read Now -

Take Ownership of Your Health: Ask Your Doctor for Your Mammograms
[]Read Now
yes-blog
yes-blog

