The Visual Verdict: DICOM vs. JPG Images in Legal Proceedings
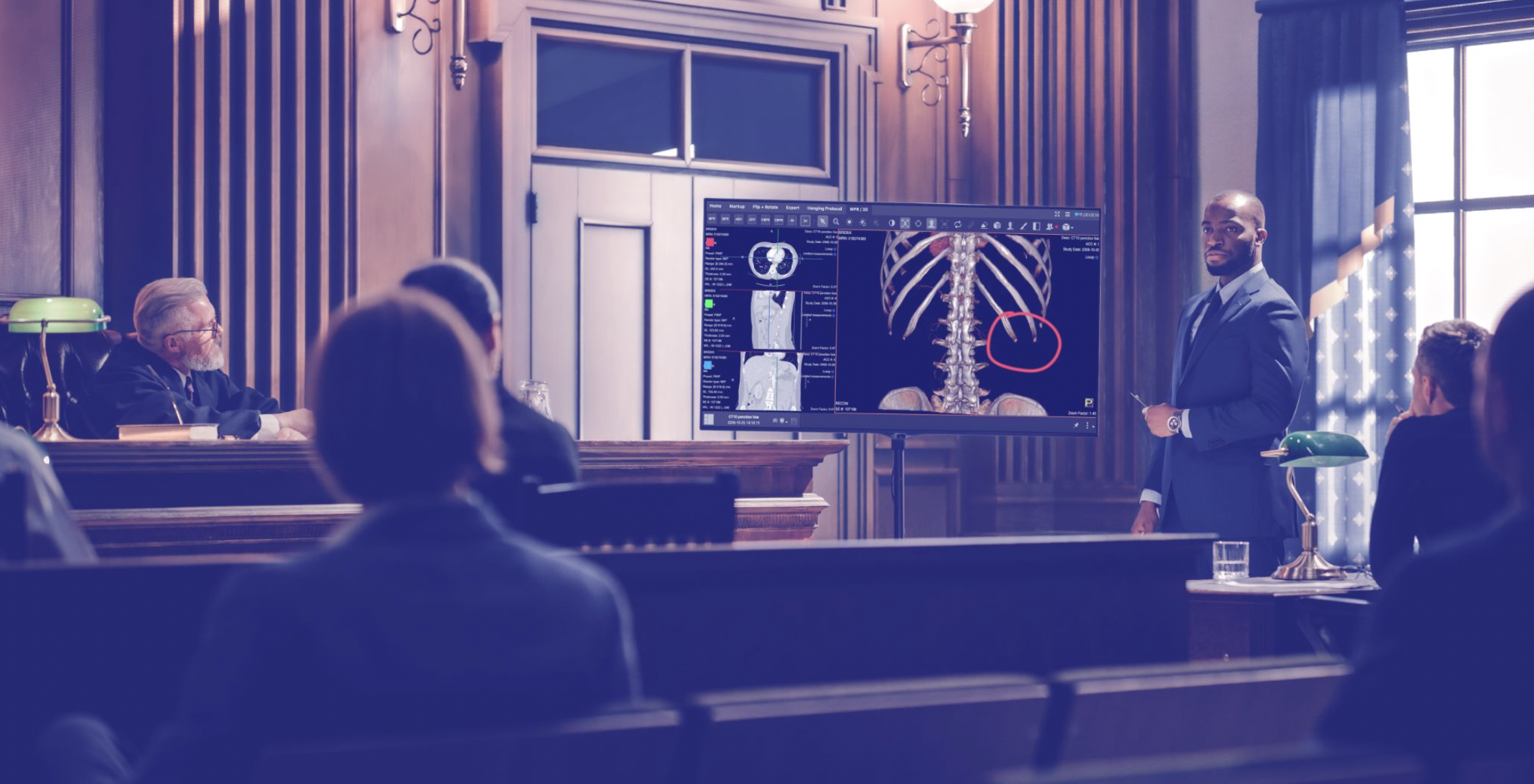
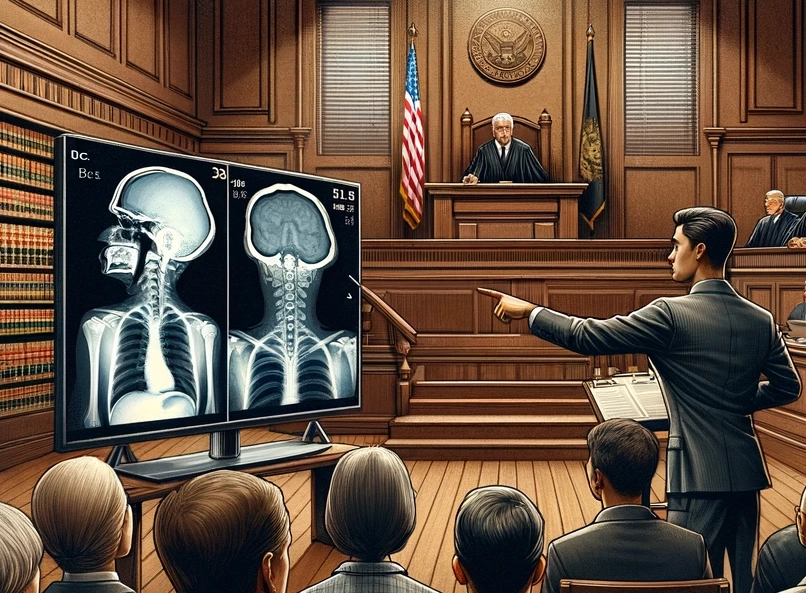
When an attorney is deciding between easy-to-handle JPG images or larger and bulkier DICOM files to illustrate their clients’ medical issues, which is better? Should you take the easy way out?
What you may not know is that the file format for these images can significantly differ, impacting their integrity and relevancy to your case. If winning your case is important to you or your client, you probably shouldn't take the easy way out.